As we discussed in our previous post, the spine supports the rest of our body. When not working optimally, our daily activities can be impeded by pain and impaired mobility. Degenerative disc disease affects the spine and is a normal part of aging. In this post, we will discuss what it is and how to treat it.
WHAT IS DEGENERATIVE DISC DISEASE?
As a result of normal aging or injury to the back, the rubbery discs that provide cushioning between the vertebrae of the spine (intervertebral discs) become weakened. These discs not only provide cushioning but also help with flexibility, allowing us to bend and twist with ease. When discs degenerate or wear down, the spine doesn’t work as efficiently. This condition is known as degenerative disc disease. It usually happens gradually, and most people aren’t aware they have it.
HOW DO YOU DIAGNOSE DEGENERATIVE DISC DISEASE?
If degenerative disc disease is suspected after a physical exam and a review of your medical history, imaging tests — X-Rays, MRI (magnetic resonance imaging), or a CT scan (computed tomography) — may be ordered to provide a better picture of the discs and bony structures of the spine.
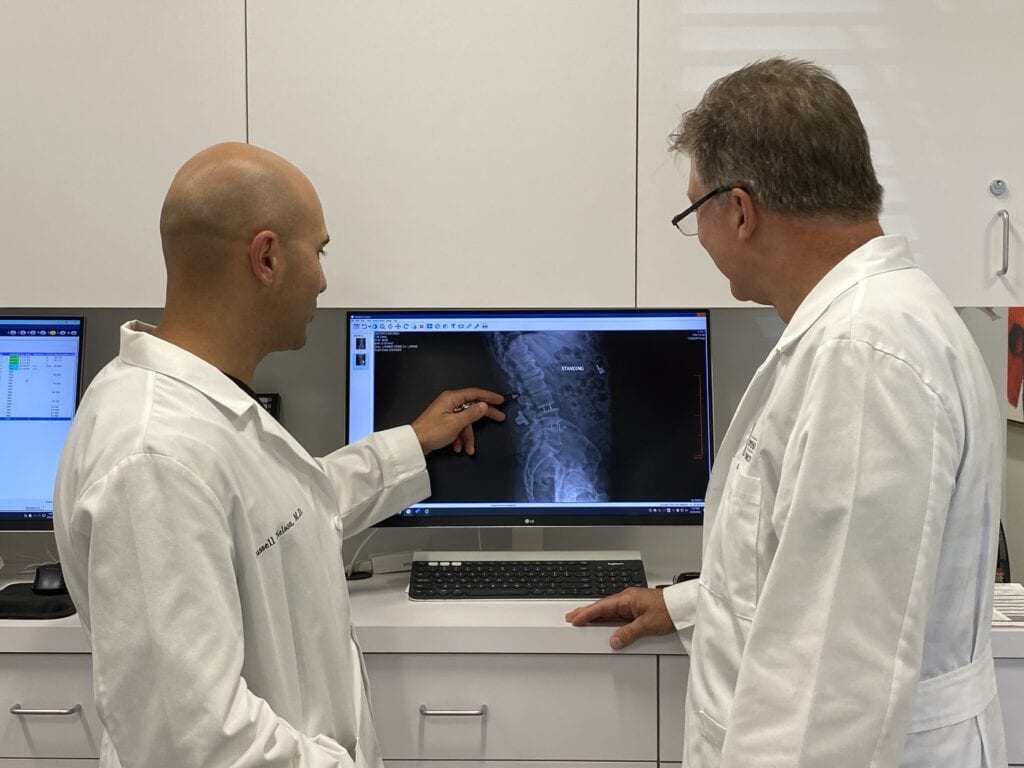
These images are not only helpful in ruling out other conditions, but if they reveal a loss of space between the discs, they can help diagnose degenerative disc disease and its severity.
WHAT HAPPENS WITH DEGENERATIVE DISC DISEASE?
Because the intervertebral discs don’t have much blood supply, they don’t repair themselves once injured. This is true whether it is a result of aging or injury.
Age – The discs can dry out and shrink as one ages.
Injury – Daily activities, sports, and injuries to the back can cause tears on the disc wall (annulus). Over time, these tears heal but scar tissue forms. This scar tissue is not as strong as the original wall. As more tears occur, more scar tissue forms, and the discs continue to weaken.
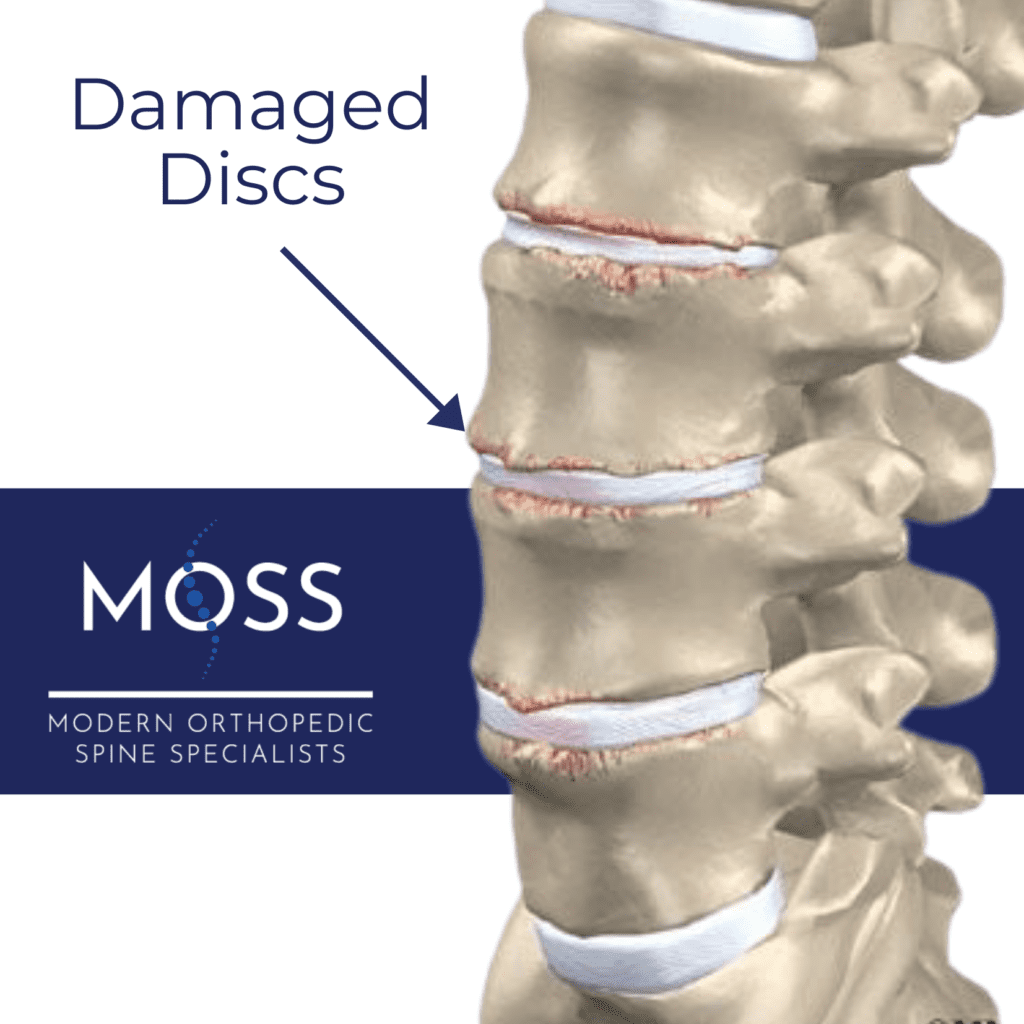
As the outer wall weakens with tears and scar tissue, the center (nucleus) of the disc loses some of its water content. The disc shrinks, and so does the space between the vertebrae. The disc can’t absorb shock as well as it once did, and the decreased space causes the joints where the vertebrae touch (facet joints) to shift unnaturally.
This shift can cause bone spurs (bony growths or osteophytes) to occur. Bone spurs aren’t always painful, but the pain does result if they pinch a spinal nerve or the spinal cord. The pain can be localized at the site of the injury, or it can cause pain, numbness, and weakness to spread from the spine to the extremity the nerve serves (radiculopathy).
Sometimes as space between the discs decreases, the openings (foramina) where the nerves exit the spine narrow. The narrowing of the foraminal canal (foraminal stenosis) can be painless, but if a nerve is compressed, it can also cause radicular pain (pain that radiates from an inflamed or compressed nerve) and radiculopathy (numbness, weakness, or neurological deficits resulting from a compressed or inflamed nerve). Pain can be nagging and constant or come and go.
CAN OTHER CONDITIONS ACCOMPANY DEGENERATIVE DISC DISEASE?
Degenerative disc disease can also cause one or more of the lower vertebrae to shift forward or backward onto the bone directly under it, resulting in a painful condition called spondylolisthesis. This shift can occur slowly over time, or it can occur suddenly. Spondylolisthesis can occur anywhere on the spine, but is most common in the lower back.
If spondylolisthesis is present with degenerative disc disease, one is more likely to be symptomatic, exhibiting one or more of these possible symptoms:
- Lower back pain – This is the most common complaint, and is often worse with exercise.
- Leg, thigh, and buttock pain – This pain worsens with standing.
- Leg pain, numbness, and tingling – This occurs if a nerve is compressed.
- Loss of bladder/bowel control (cauda equina syndrome) – If more severe nerve compression is present.
- Hamstring tightness and stiffness.
SHOULD I BE CONCERNED IF I HAVE DEGENERATIVE DISC DISEASE?
Most people will experience at least some degree of degenerative disc disease as they age, but it is not always a cause for concern. If you don’t have symptoms, there is normally no reason to treat it. If, however, you experience symptoms, therapy and some sort of intervention may be warranted (depending on the symptoms and their severity).
Here at MOSS, we recognize that each individual is unique and will present with different needs. We treat the patient and not the imaging.
If symptoms are present, they are usually experienced in the neck and lower back. Pain is the most common symptom and may:
- Come and go.
- Radiate from the lower back to the buttocks and thighs.
- Range from mild to disabling.
- Extend to the arms, hands, or legs and feet.
- Increase with movements such as sitting, bending, twisting, or lifting.
- Be relieved by moving, walking, and/or lying down.
Sometimes numbness and tingling are present, along with muscle weakness. If that is the case, nerve compression might be present.
WHAT ARE SOME TREATMENTS FOR DEGENERATIVE DISC DISEASE?
As we mentioned earlier, if no symptoms are present, generally no treatment is necessary. However, if symptoms are present, our goal is to decrease your pain and halt further damage. We will discuss with you your options, and together we’ll decide on those treatment options which will work best for you. We usually recommend non-invasive therapies first, and only progress to more invasive if needed:
- Medication – Over-the-counter pain relievers, like Tylenol or ibuprofen and other NSAIDs (nonsteroidal anti-inflammatory drugs), may help in relieving pain and reducing inflammation.
- Supplements — Glucosamine and Chondroitin, turmeric, and Omega-3s are among some supplements that may reduce inflammation and improve joint health, especially if used for longer periods of time.
- Physical therapy – Certain exercises, stretches, and movements that help strengthen the muscles that support your neck and spine can be very helpful in alleviating pain and decreasing symptoms.
- Heat and cold therapy – This is especially helpful if the degenerative disc disease is a result of a recent injury.
- Corticosteroid injections – These injections into the epidural space help to decrease inflammation and pain.
- Surgery – If all other treatment options are ineffective at reducing pain and symptoms, surgery might be recommended.
WHAT ARE SOME SURGICAL OPTIONS FOR DEGENERATIVE DISC DISEASE THAT HAS NOT RESPONDED TO OTHER OPTIONS?
Here at MOSS, we prefer the least invasive options because that means a quicker recovery for you, while still providing optimal results and pain relief.
OLIF — Oblique Lateral Interbody Fusion is a minimally invasive surgical technique that involves a minor incision that we use to access and repair the spine. After years of research and practice, you can be confident Dr. Oganesian will provide you with the best care possible.
OLIF is a good option for treating degenerative disc disease (with or without spondylolisthesis) that is causing pain and is unresponsive to other therapies.
Endoscopic Foraminotomy — This is also a minimally invasive technique used to enlarge the openings (foramina) for the nerve roots so that compression is relieved, thereby eliminating the symptoms caused by foraminal stenosis (narrowing of the nerve openings in your spine).
Aging and injury don’t have to stop you from doing the things you love. Dr. Armen Oganesian and his highly skilled team are dedicated to helping you return to optimal functioning with minimal intervention.
For an individual consultation, contact Dr. Arman Oganesian at The Modern Spine Specialists today! Please contact The Modern Spine Specialists at 805-370-0748, or email us at info@themodernspine.com.
You can also visit our office at:
250 Lombard Street
Thousand Oaks, CA 91360

Recent Comments